The Sports Medicine Patient Advisor serves as a comprehensive guide, empowering patients with knowledge to manage injuries and communicate effectively with healthcare providers, ensuring optimal recovery and safe return to activity.
1.1 Overview of the Guide
The Sports Medicine Patient Advisor is a comprehensive resource designed to assist patients, athletes, coaches, and healthcare providers in managing sports-related injuries and rehabilitation. It offers detailed handouts, exercise programs, and return-to-play protocols, ensuring a holistic approach to recovery. The guide bridges the communication gap between patients and medical professionals, empowering individuals to actively participate in their care. With a focus on evidence-based practices, it covers various injuries, preventive strategies, and rehabilitation techniques. The Advisor serves as an essential tool for anyone seeking to understand and navigate the complexities of sports medicine, ensuring safe and effective return to activity.
1.2 Importance of Patient Education in Sports Medicine
Patient education is crucial in sports medicine as it equips individuals with the knowledge to actively participate in their care, fostering better outcomes and adherence to treatment plans. By understanding their diagnoses, patients can make informed decisions, reducing recovery times and minimizing complications. Effective communication between patients and healthcare providers ensures personalized care, addressing specific needs and concerns. The Sports Medicine Patient Advisor emphasizes this by providing clear, accessible information, enabling patients to take ownership of their health. This collaborative approach not only enhances recovery but also strengthens the patient-provider relationship, ultimately leading to safer and more successful returns to activity and sport.
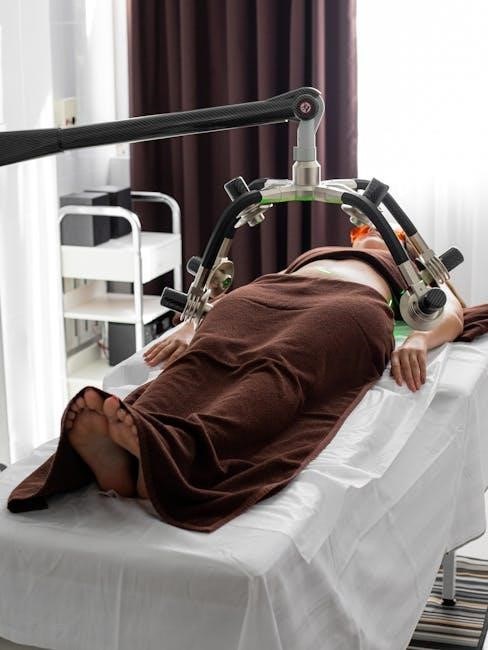
Key Concepts in Sports Medicine
Sports medicine focuses on understanding, preventing, and treating injuries, optimizing performance, and promoting recovery. It integrates medical care, rehabilitation, and education to ensure safe return to activity and sport.
2.1 Understanding Sports Injuries and Rehabilitation
Understanding sports injuries and rehabilitation is crucial for effective recovery and return to activity. Sports injuries vary in severity, from minor strains to complex tears, often requiring personalized treatment plans. Rehabilitation involves a structured approach, including rest, physical therapy, and gradual reintroduction of movement. Early intervention and proper diagnosis are key to preventing long-term damage; Patient education plays a vital role, empowering individuals to adhere to rehabilitation protocols and avoid re-injury. The process also emphasizes strengthening, flexibility, and pain management to restore function and performance. A well-designed rehabilitation plan ensures athletes safely progress, achieving optimal recovery and readiness for their sport or activity. Consistency and adherence to medical advice are essential for successful outcomes.
2.2 The Role of the Sports Medicine Patient Advisor
The Sports Medicine Patient Advisor acts as a bridge between patients and healthcare providers, ensuring clear communication and understanding of diagnoses and treatment plans. This role involves providing educational resources, such as handouts and guidelines, to empower patients with knowledge about their injuries and recovery processes. The advisor also helps patients navigate rehabilitation programs, offering practical advice on exercises, nutrition, and lifestyle adjustments. By fostering collaboration between patients and their medical teams, the advisor ensures personalized care and optimal outcomes. Their expertise enables patients to make informed decisions, adhere to treatment plans, and achieve a safe and effective return to their sport or activity. This role is essential for improving patient engagement and overall healthcare outcomes in sports medicine.

Common Sports-Related Injuries
Common sports injuries include knee injuries, rotator cuff strains, low back pain, and plantar fasciitis. These injuries often result from overuse or trauma, requiring targeted treatment and rehabilitation.
3.1 Knee Injuries: Causes, Symptoms, and Treatment
Knee injuries are common in sports, often caused by overuse, sudden stops, or direct trauma. Symptoms include pain, swelling, and limited mobility. Treatment involves RICE (rest, ice, compression, elevation) and physical therapy; Severe cases may require surgery, followed by rehabilitation to restore strength and flexibility, ensuring a safe return to activity.
3.2 Rotator Cuff Injuries: Diagnosis and Management
Rotator cuff injuries involve strains or tears in the tendons of the shoulder, often caused by overuse, falls, or direct trauma. Symptoms include shoulder pain, weakness, and limited arm movement. Diagnosis typically involves physical exams, imaging tests like MRI or X-rays, and strength assessments. Management strategies include rest, ice, physical therapy, and anti-inflammatory medications. Severe tears may require surgical intervention, followed by rehabilitation to restore strength and mobility. Early diagnosis and appropriate treatment are crucial to prevent further damage and ensure a successful recovery, enabling patients to regain functional use of their shoulder and return to their normal activities safely.
3.3 Low Back Pain in Athletes
Low back pain is a common issue among athletes, often resulting from repetitive stress, poor posture, or direct injury. It manifests as pain and stiffness in the lower back, sometimes radiating to the legs. Causes include muscle strains, herniated discs, or overuse. Diagnosis involves physical exams and imaging to rule out serious conditions. Management focuses on rest, stretching, and strengthening exercises. Anti-inflammatory medications may alleviate symptoms, while physical therapy can improve core stability and posture. Addressing underlying issues is key to preventing recurrence and ensuring a safe return to sports. Early intervention and proper rehabilitation strategies help athletes regain functionality and minimize downtime, promoting long-term spinal health and performance.
3.4 Plantar Fasciitis: Prevention and Recovery
Plantar fasciitis is a painful inflammation of the plantar fascia, often caused by overuse or improper footwear. Prevention involves wearing supportive shoes, using orthotics, and stretching the Achilles tendon and plantar fascia. Strengthening exercises for the foot and calf muscles can also reduce risk. Recovery strategies include rest, ice therapy, and anti-inflammatory medications to alleviate symptoms. Gentle stretching and physical therapy exercises are recommended to promote healing and restore flexibility. Avoiding high-impact activities during recovery is crucial to prevent re-injury. In severe cases, corticosteroid injections may be necessary. Consistent adherence to preventive and recovery measures ensures a faster return to activity while minimizing the likelihood of recurrence, promoting long-term foot health and function.

Rehabilitation and Recovery Strategies
Effective rehabilitation focuses on restoring strength, flexibility, and function, ensuring a safe return to sports. Tailored exercises, progressive loading, and patient education are key components for optimal recovery.
4.1 Early versus Delayed Lengthening Exercises for Hamstring Injuries
Research highlights the debate between early and delayed lengthening exercises for hamstring injuries. Early intervention, starting within 48-72 hours post-injury, promotes faster recovery by reducing scar tissue and improving flexibility. Delayed exercises may prolong recovery, increasing the risk of chronic tightness. A randomized controlled trial found that athletes who began early lengthening exercises returned to sport sooner, with reduced reinjury rates. The study emphasizes the importance of gradual progression and proper technique to avoid overloading the hamstrings. This approach aligns with rehabilitation goals, ensuring a safe and efficient return to activity while minimizing long-term complications.
4.2 The Goal of Rehabilitation: Safe Return to Sport
The primary goal of rehabilitation is to ensure a safe and effective return to sport, minimizing the risk of reinjury. This involves a structured approach, focusing on strength, flexibility, and functional recovery. Patients must meet specific criteria, such as achieving pre-injury performance levels and demonstrating injury-free participation in practice. Rushing back to sport can lead to prolonged recovery or chronic issues. Rehabilitation plans are tailored to individual needs, ensuring athletes regain necessary skills and confidence. The process emphasizes gradual progression, with continuous monitoring by healthcare providers to confirm readiness. A safe return to sport is achieved when the athlete can perform without pain or limitations, ensuring long-term health and performance.

Communication Between Patients and Healthcare Providers
Effective communication is crucial for understanding diagnoses and treatment plans. The Sports Medicine Patient Advisor helps bridge gaps, ensuring patients actively participate in their care and recovery journey.
5.1 Bridging the Gap in Understanding Diagnoses and Treatment Plans
The Sports Medicine Patient Advisor plays a vital role in improving patient-provider communication by simplifying complex medical information. It provides clear explanations of diagnoses, treatment options, and recovery processes, ensuring patients understand their conditions and the rationale behind recommended therapies. By offering detailed yet accessible content, the guide empowers patients to ask informed questions and engage actively in decision-making. This resource also helps healthcare providers deliver consistent and patient-centered care, fostering trust and collaboration. The Advisor’s structured approach ensures that both patients and providers are aligned, reducing misunderstandings and enhancing overall outcomes. Its comprehensive handouts and easy-to-understand language make it an invaluable tool for effective communication in sports medicine.
5.2 Empowering Patients to Participate in Their Healthcare Journey
The Sports Medicine Patient Advisor is designed to empower patients by providing them with the knowledge and tools necessary to take an active role in their healthcare. By offering clear, concise information about diagnoses, treatment options, and recovery processes, the guide enables patients to make informed decisions. It encourages open communication with healthcare providers, fostering a collaborative approach to care. The Advisor also includes practical tips and resources, such as exercise programs and nutrition advice, to support patients in managing their conditions effectively. This empowerment not only enhances patient satisfaction but also leads to better health outcomes and a smoother transition back to sports and daily activities.

Exercise and Activity Guidelines
Exercise and activity guidelines in The Sports Medicine Patient Advisor provide structured programs for injury recovery, ensuring a safe and gradual return to sports and physical activities.
6.1 Exercise Programs for Injury Recovery
The Sports Medicine Patient Advisor outlines structured exercise programs tailored to specific injuries, promoting gradual recovery and strength restoration. These programs emphasize a balance between rest and controlled movement to prevent further damage. By incorporating stretching, strengthening, and flexibility exercises, individuals can address muscle imbalances and improve joint stability. The guide also highlights the importance of progression, ensuring exercises adapt as the patient heals. Monitoring progress and adjusting routines are key to achieving optimal results. The ultimate goal is to restore function and prepare the body for a safe return to activity, minimizing the risk of re-injury while enhancing overall performance and well-being.
6.2 Return-to-Play Protocols
The Sports Medicine Patient Advisor provides detailed return-to-play protocols to ensure athletes safely resume their activities after injury. These protocols are tailored to individual recovery progress, emphasizing gradual reintegration into sports. Criteria for clearance include pain levels, strength, flexibility, and functional testing. The guide stresses that return to play should not be based on time elapsed but on the body’s readiness. By adhering to these structured protocols, athletes minimize the risk of re-injury and achieve a successful transition back to their sport. The Advisor’s guidelines empower healthcare providers and athletes to make informed decisions, ensuring a safe and effective return to activity.
Preventive Strategies in Sports Medicine
The Sports Medicine Patient Advisor emphasizes preventive strategies, including proper nutrition, strengthening exercises, and conditioning programs, to minimize injury risks and enhance athletic performance effectively.
7.1 The Role of Nutrition in Injury Prevention
Nutrition plays a crucial role in injury prevention by ensuring optimal energy levels, supporting muscle repair, and maintaining immune function. A balanced diet rich in proteins, carbohydrates, and essential vitamins helps athletes build resilience against injuries. Adequate hydration is also vital to prevent muscle cramps and maintain joint health. Additionally, antioxidants and omega-3 fatty acids can reduce inflammation, which is often associated with sports-related injuries. Proper fueling before and after workouts enhances performance and accelerates recovery. The Sports Medicine Patient Advisor provides detailed guidance on creating personalized nutrition plans tailored to specific sports and athlete needs, emphasizing the importance of nutrition in overall injury prevention strategies.
7.2 Strengthening and Conditioning Programs
Strengthening and conditioning programs are essential for injury prevention and enhancing athletic performance; These programs focus on building muscle strength, endurance, and flexibility, while improving coordination and balance. By addressing muscle imbalances, they reduce the risk of overuse injuries and enhance overall resilience. Tailored to an athlete’s specific sport or position, these programs often include exercises targeting core stability, plyometrics, and functional movements. Proper progression and periodization ensure gradual adaptation, minimizing the risk of overtraining. The Sports Medicine Patient Advisor emphasizes the importance of structured conditioning plans, highlighting their role in maintaining long-term health and optimizing performance. Regular participation in such programs can significantly lower injury rates and improve recovery capabilities for athletes at all levels.
The Role of Medications in Sports Medicine
Medications, such as NSAIDs, play a crucial role in managing pain and inflammation in sports injuries, enabling athletes to recover and return to activity safely and effectively.
8.1 Use of Non-Steroidal Anti-Inflammatory Drugs (NSAIDs)
NSAIDs are widely used in sports medicine to manage pain, inflammation, and swelling associated with injuries. These medications, such as ibuprofen and naproxen, work by inhibiting the production of prostaglandins, which contribute to inflammation. They are commonly prescribed for acute injuries, chronic conditions like tendinitis, and post-surgical recovery. While effective, NSAIDs should be used cautiously, as prolonged use can lead to gastrointestinal side effects and other complications. It is essential to follow recommended dosages and consult a healthcare provider to ensure safe and appropriate use. NSAIDs do not cure injuries but help alleviate symptoms, allowing athletes to participate in rehabilitation and return to activity more comfortably.

Special Considerations for Specific Populations
The Sports Medicine Patient Advisor addresses the unique needs of specific populations, including pregnant athletes and young competitors, ensuring safe and tailored approaches to injury management and recovery.
9.1 Exercise During Pregnancy and Postpartum Period
Exercise during pregnancy and the postpartum period is crucial for maintaining physical fitness and reducing complications. Guidelines from the American College of Obstetricians and Gynecologists emphasize moderate aerobic and strength training activities, avoiding high-risk maneuvers. The Sports Medicine Patient Advisor provides tailored recommendations, ensuring safe participation and recovery. Benefits include improved cardiovascular health, reduced gestational diabetes risk, and faster postpartum recovery. However, activities must be personalized based on trimester, medical history, and physical condition. Healthcare providers play a key role in designing programs that balance safety and effectiveness, empowering women to maintain an active lifestyle throughout pregnancy and beyond, fostering overall well-being for both mother and baby.
The Sports Medicine Patient Advisor is a vital resource, empowering patients and healthcare providers with comprehensive tools for optimal care, fostering effective communication and successful recovery outcomes.
10.1 The Impact of The Sports Medicine Patient Advisor on Patient Care
The Sports Medicine Patient Advisor has revolutionized patient care by bridging communication gaps between patients and healthcare providers. It empowers patients with actionable knowledge, enabling them to actively participate in their recovery journey. By providing clear, evidence-based information, the guide ensures patients understand their diagnoses, treatment options, and rehabilitation processes. This enhanced understanding fosters trust and collaboration, leading to better adherence to treatment plans. The Advisor’s comprehensive handouts, exercise programs, and return-to-play protocols serve as invaluable tools for healthcare providers, ultimately improving patient outcomes. Its holistic approach ensures safer and more effective recoveries, making it an indispensable resource in modern sports medicine.
